Psilocybin-assisted therapy could help a wide range of people suffering from depression, based on a recent randomized clinical trial. Psilocybin combined with psychotherapy might also be better than psychotherapy or pharmaceuticals on their own. So, as more clinical trials are conducted, the number of people potentially helped by psilocybin-assisted therapy is likely to continue to expand.
Psilocybin-assisted Therapy Might Help a Wide Range of People
Psilocybin-assisted therapy might help people suffering from major depressive disorder (MDD), according to a recent randomized clinical trial in the medical journal JAMA Psychiatry. The study found that “psilocybin-assisted therapy was efficacious in producing large, rapid, and sustained antidepressant effects in patients with major depressive disorder” [1].
In contrast to earlier psilocybin studies focusing only on depression which was treatment-resistant or in terminal cancer patients, Davis and colleagues showed that psilocybin-assisted therapy could help a wide range of people suffering from depression. This is a significant step forward in psilocybin research. An editorial in the same issue of JAMA Psychiatry said that more research is necessary. But psilocybin at least has “potential for more generalized clinical use” [4].
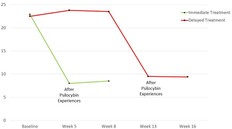
Current study participants were put into random groups. Two groups received psilocybin experiences at different times. The immediate-treatment group received psilocybin in weeks 3 and 4. Meanwhile the delayed-treatment group received in weeks 11 and 12. However, in weeks 5 and 8, the GRID-Hamilton scale assessed severity of depression ratings for both groups. The delayed-treatment group received a severity of depression rating in weeks 13 and 16.
In weeks 5 and 8, the immediate-treatment group had “significantly lower depression scores” [1] compared to the delayed-treatment group. After the delayed-treatment group’s own psilocybin experiences, its depression scores were also significantly lower.
Lower Depression Scores (Mean) After Psilocybin Experiences
Based on data from Davis et al.
Pharmacotherapy and Psychotherapy
Many studies have pointed toward the possible benefits of combining pharmacotherapy and psychotherapy rather than pursuing each treatment on its own [1]. Davis et al showed similar results with psilocybin-assisted therapy, “The effect sizes reported in this study were approximately 2.5 times greater than the effect sizes found in psychotherapy and more than 4 times greater than the effect sizes found in psychopharmacological depression treatment studies” [1]. Davis et al also wrote that the seemingly low adverse effects of psilocybin compared to some antidepressant medications could make psilocybin an attractive option to both patients and therapists.
The research team also claimed that psilocybin experiences might have longer-lasting therapeutic benefits. Compare this to a single infusion of ketamine: “…ketamine effects typically last for a few days to 2 weeks, whereas the current study showed that clinically significant antidepressant response to psilocybin therapy persisted for at least 4 weeks” [1]. However, note that Davis et al were referring to results after one infusion of ketamine. Whereas, some ketamine therapists recommend multiple infusions over multiple days. In addition, Davis et al cited evidence that psilocybin has a lower potential for addiction than ketamine [2].
4 Stage Process
Davis’ therapy format followed a four-stage process that has now become a standard in studies of psilocybin-assisted therapy [3]. Thus, these stages are: assessment, preparation, experience, and integration.
870 candidates went through the assessment phase of the current study. This eventually narrowed to 27 participants. Meanwhile, candidates were deemed ineligible for a variety of criteria. This includes current use of antidepressant medications, a recent history of substance abuse, or a medically significant suicide attempt. 24 participants eventually completed all of the psilocybin experiences plus post-experience integrations.
Preparation involved 8 hours of meetings with 2 session facilitators for 3 weeks prior to the first psilocybin experience. In the first experience, participants took a psilocybin dose of 20 milligrams per 70 kilograms of body weight. The dose in the second experience was 30 milligrams per 70 kilograms of body weight, considered a high psilocybin dose. So each experience lasted several hours over the course of one day.
Participants lay down for most of the experience in a “living room-like environment” [1] while wearing eyeshades and listening to music. Facilitators were in the room with participants and encouraged “participants to focus their attention inward and stay with any experience that arose” [1]. After that, over the following weeks, two integration sessions were held for participants to discuss their experiences with the facilitators. Lastly, participants were rated for depression severity during these integration sessions.
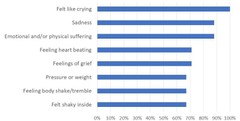
To sum up, Davis et al reported that there “were no serious adverse events in this trial” [1]. However, future participants and facilitators should be aware that the sessions were not without difficulties, and a number of “nonserious” adverse effects were reported:
Nonserious Adverse Effects (1st Psilocybin Experience)
Based on data from Davis et al.
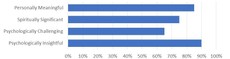
Top 5 Most Important Life Experience
However, most participants also ranked their psilocybin experiences as among the top 5 most important of their lives. Many even ranked them as the MOST important of their lives.
Psilocybin Experiences Ranked as
Top 5 Most Important Ever…
Based on data from Davis et al.
Psilocybin-Assisted Therapy Might Help You
As research continues expanding to more medical conditions, so could a consensus that psilocybin-assisted therapy might help a wide range of people. A variety of clinical trials are being conducted about psilocybin and other psychedelics. Studies are currently being conducted about psilocybin’s potential to help treat anorexia nervosa, nicotine addiction, and Alzheimer’s Disease. It’s too soon to say how these studies will turn out. But the future might be promising for the psilocybin community.
References
1. Davis, A., Barrett, F., May, D., et al. (2020). Effects of Psilocybin-Assisted Therapy on Major Depressive Disorder A Randomized Clinical Trial. JAMA Psychiatry, online, 4 Nov. 2020, https://jamanetwork.com/article.aspx?doi=10.1001/jamapsychiatry.2020.3285
2. Johnson, M., Griffiths, R., Hendricks, P., & Henningfield, J. (2018). The Abuse Potential of Medical Psilocybin According to the 8 Factors of the Controlled Substances Act. Neuropharmacology, 142, 143-166. https://doi.org/10.1016/j.neuropharm.2018.05.012
3. Nutt, D., Carhart-Harris, R. (2020). The Current Status of Psychedelics in Psychiatry. JAMA Psychiatry, online, 29 July 2020, https://doi.org/10.1001/jamapsychiatry.2020.2171
4. Reynolds, C. (2020). Psilocybin-Assisted Supportive Psychotherapy in the Treatment of Major Depression—Quo Vadis? JAMA Psychiatry, online, 29 July 2020, https://doi.org/10.1001/jamapsychiatry.2020.2171
Photo by Pablo Heimplatz on Unsplash