Dan is beaming as he declares, “Dang, you’re so beautiful! Does your man know how lovely you are?” Dan’s wearing a T-shirt and shorts, but it’s the middle of winter. He’s talking fast and gesticulating wildly as he tells me about his new discoveries in sacred geometry.
I’ve only met Dan once before and our interaction at the time was brief and professional, so I’m a little taken aback by his intimate tone with me now. But as a healthcare provider, I also understand what’s going on: Dan is showing signs of mania, a state characterized by elevated mood, hyperactivity, and a reduced need for sleep. Mania is commonly seen in people with Bipolar 1 Disorder (formerly known as manic depression), though manic states can also be seen in those without the condition.
Extended periods of sleep deprivation, major stressors such as the death of a loved one, and childbirth in women can all trigger manic states. Drugs, too, can bring on mania. This includes both pharmaceutical medications, like some anti-depressant drugs, as well as psychedelics. It’s for this reason that those with a personal history or a strong family history of Bipolar 1 or psychosis (like schizophrenia) are advised to avoid using psychedelics altogether or, at least from a harm reduction standpoint, to use very high levels of caution when taking substances like LSD, psilocybin, and ayahuasca.
Too Much Medicine
Shortly after bumping into Dan, I called a mutual friend of ours, Matthew. He explained that Dan had been drinking ayahuasca on an almost weekly basis, in spite of several friends expressing their concerns and asking him to take a break.
Unsurprisingly, Dan ended up in the hospital a few days later, and I found myself feeling very angry. Not with this bright-eyed, cavalier young man who was trying to get a handle on his early childhood trauma, but rather with the medicine carrier that kept serving him ayahuasca week after week, even after – I learned from Matthew – Dan began showing signs of mania. I think most people would agree that Dan’s story is an unfortunate one. And while I do not doubt that there were some positive elements to Dan’s breakdown, I also think this episode did Dan more harm than good in both the short and long term.
Now, having a manic episode or even a psychotic break can be a powerful, meaningful experience for some people, but it is by no means the only path, nor the ideal one. There are a myriad of safer ways to learn, grow, and awaken without having to end up in the hospital or seriously freak out one’s friends and family.
Psychosis and Psychedelics Don’t Always Mix Well
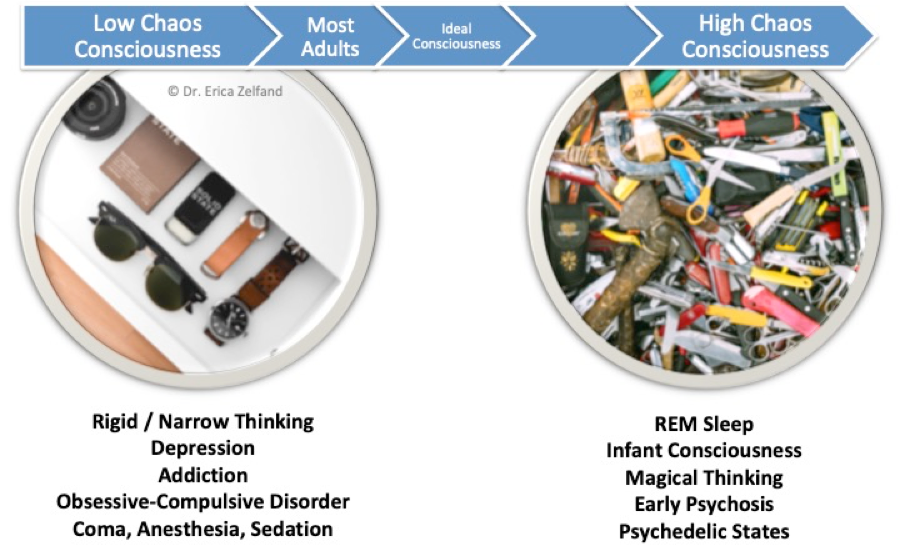
Part of how psychedelics work is by increasing the amount of entropy, or chaos, in the brain. In fact, in a paper titled, “The Entropic Brain: A Theory of Conscious States Informed by Neuroimaging Research with Psychedelic Drugs,” neuropsychopharmacologist Dr. Robin Carhart-Harris and his co-authors explore this very nature of psychedelics [1]. They propose that conditions like depression, obsessive-compulsive disorder (OCD), and addiction result from too much order, or rigidity, in certain parts of the brain. Psychedelics, they argue, may help heal these conditions by disrupting that rigidity, through a mechanism much like shaking a snow globe.
Psychedelics appear to disrupt the neural patterns upon which rigid patterns of thought and behavior – such as those seen in depression, OCD, and addiction – rest. The accompanying graphic, which I’ve adapted from a similar image found in Carhart-Harris’ paper, shows how some of us are on the rigid, or low chaos, end of the consciousness spectrum, and some of us are more on the entropic, or high chaos end.
If we think of psychosis and mania as high chaos states, we can see how taking a chaos-increasing medicine like LSD might just push someone with a propensity towards mania or psychosis over the edge. When a patient’s brain is in the middle of a blizzard, after all, they don’t need their metaphorical snow globe shaken. Dr. Carhart-Harris and his team have also performed other studies in which the brain scans of people on psychedelics were compared to baseline images [2]. This work reveals that psychedelics enhance neural crosstalk – the phenomenon by which novel connections are made between parts of the brain that don’t normally communicate with one another.
More Neural Networking
The following is a simplified illustration of the neural connections tracked in the brains of study participants upon receiving placebo (a) vs. psilocybin (b). The participants who received psilocybin were observed to have many more neural connections than those who received a placebo [3].
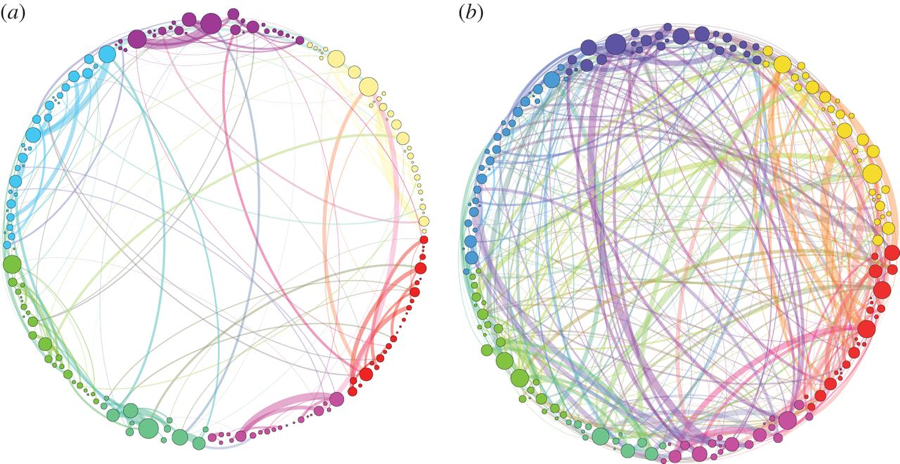
Someone with depression whose thoughts are focused on a very tight loop of negative, self-denigrating sentiments may very well benefit from a little increased cross-talk. More neural connections might allow them to realize that life can actually be pretty awesome (or at least bearable), and that so many things are interconnected. They may realize that it’s not so scary after all to take the risk of asking somebody out on a date, to read more about geometry, science, or self-growth, or to spend a little money on a stylish new haircut.
Someone in a manic or psychotic state, however, doesn’t need a nudge in that direction. In fact, they’re already at high risk of seeing synchronicity where there is none, being overly familiar (as Dan was with me), becoming obsessed with fractals (or whatever has caught their interest), and racking up credit card debt in the pursuit of whimsies. It is perhaps for these reasons that most, if not all, of the studies on psychedelic medicine exclude those with a personal history of Bipolar 1 or psychosis from enrolling.
Right Medicine, Right Condition, Right Time
We are all hopefully able to stay aware of our connection with reality and give our bodies and brains the support they need. When that fails, however, that’s where our friends, families, and mental health professionals can help us out. This is also when it’s time for medicine carriers to have frank conversations with their guests, connect them with mental health resources, and refuse to serve them more medicine until they’re grounded again (if ever).
When psychedelic users begin losing touch with reality, going days without sleeping, and showing other signs of mania or psychosis, the answer isn’t more chaos-inducing medicine. The answer, more often than not, is rest, sobriety (including a break from sacred medicines like rapé), re-grounding, integration therapy, community support, and/or self-reflection.
If researchers and practitioners in this emerging area continue to think of psychedelics as medicines, it’s easy to see that as with all medicines, psychedelics are not appropriate for every situation. Antibiotics, for example, have saved countless lives due to their ability to combat bacterial invasion. But, as they can only fight bacteria, they are completely useless in the milieu of viral or fungal infections. Antibiotics also carry risks, such as disruption of the microbiome (the diversity and balance of good and bad microbes in the gut), and most concerning of all, they contribute to antibiotic-resistant superbugs. Antibiotics are not the appropriate solution to every kind of infection. So why, then, would we think that psychedelics could be the right medicine for every kind of mental/emotional ailment? Every medicine has its indications, and every therapy comes with risk.
Know When to Say “No”
When individuals begin showing signs that they’re losing touch with reality, it’s usually a sign that it’s time to take a break from psychedelic use. It’s also likely time to work with a therapist or integration counselor to make sense of what occurred and find any wisdom to be gleaned, to cut back on work and social obligations, to rest, to connect with loved ones, to spend time in nature, and to get both feet firmly rooted – both physically and psychologically – back here on Earth.
You can’t launch into outer space, after all, without good ground control. And some of us – whether it’s due to social circumstances, genetics, or medical influences – just don’t have good ground control. And that’s ok. There are other medicines, other therapies, and other pathways to insight, growth, and healing.
Follow your Curiosity
Sign up to receive our free psychedelic courses, 45 page eBook, and special offers delivered to your inbox.References
- Carhart-Harris, Robin Lester, Robert Leech, Peter John Hellyer, Murray Shanahan, Amanda Feilding, Enzo Tagliazucchi, Dante R. Chialvo, and David Nutt. “The entropic brain: a theory of conscious states informed by neuroimaging research with psychedelic drugs.” Frontiers in human neuroscience 8 (2014): 20.
- Carhart-Harris, Robin L., Suresh Muthukumaraswamy, Leor Roseman, Mendel Kaelen, Wouter Droog, Kevin Murphy, Enzo Tagliazucchi, et al. “Neural correlates of the LSD experience revealed by multimodal neuroimaging.” Proceedings of the National Academy of Sciences 113, no. 17 (2016): 4853-4858.
- Petri, Giovanni, Paul Expert, Federico Turkheimer, Robin Carhart-Harris, David Nutt, Peter J. Hellyer, and Francesco Vaccarino. “Homological scaffolds of brain functional networks.” Journal of The Royal Society Interface 11, no. 101 (2014): 20140873.